37-year-old gentleman came with the complaints of cough, breathlessness with mild fever on/off since 1 month
- A 37-year-old gentleman came with complaints of cough, breathlessness with mild fever on/off for 1 month
- Below are the HRCT images of the patient
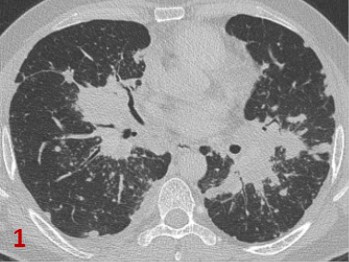
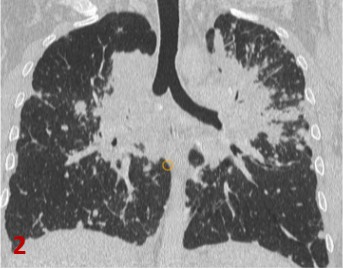
Fig 1 Axial CT and Fig 2 Coronal CT in lung window: Confluent areas of consolidations and fibrotic opacities(*) with spiculated margins in perihilar regions of both lungs predominantly involving upper lobes .
Diffuse micro nodular and coalescent macro nodular opacities ( large arrows) seen along peribronchovascular distribution in both lung parenchyma.
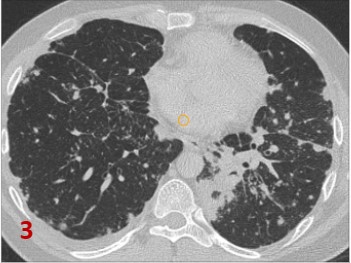
Fig 3 Axial CT in lung window: Multiple subpleural, fissural and septal nodules (line arrows)in both lungs with reticular opacities, fissural and pleural thickening.
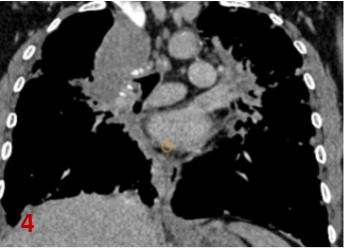
Fig 4 Coronal CT in soft tissue window: Multiple prominent mediastinal lymph nodes (curved arrows) in pretracheal, paratracheal, subcarinal and bilateral hilar regions with amorphous calcifications within.
DIAGNOSIS:
Pulmonary Sarcoidosis.
- Bronchoalveolar lavage- lymphocytosis, CD4/CD8 ratio >3.5
- EBUS-TBNA for sampling mediastinal adenopathy- non necrotising granulomas.
- Transbronchial Lung biopsy.
- Mediastinoscopy.
- Serology- ACE and sIL-2R levels
DIFFERENTIAL DIAGNOSIS ( on HRCT)
- Tuberculosis- Asymmetric Necrotic mediastinal nodes, cavitations, centrilobular or randomly distributed nodules.
- Chronic beryllium disease and Silicosis- egg shell calcification of lymphnodes.
- Sarcoid-like reaction in malignancy, drug reaction and medical device implantation.
DISCUSSION:
- Sarcoidosis is a multisystem disorder that is characterized by noncaseous epithelioid cell granulomas, which may affect almost any organ.
- Thoracic involvement is common and accounts for most of the morbidity and mortality associated with the disease.
- Thoracic radiologic abnormalities are seen at some stage in approximately 90% of patients with sarcoidosis, and an estimated 20% develop chronic lung disease leading to pulmonary fibrosis.
HRCT findings of Pulmonary sarcoidosis
- Typical features
- Lymphadenopathy: hilar, mediastinal (right paratracheal), bilateral, symmetric, and well defined.
- Nodules: micronodules (2–4 mm in diameter; well defined, bilateral); macronodules (≥5 mm in Diameter, coalescing)
– Lymphangitic spread: peribronchovascular, subpleural, interlobular septal nodules.
– Fibrotic changes: reticular opacities, architectural distortion, traction bronchiectasis, bronchiolectasis, volume loss.
– Bilateral perihilar opacities: Predominant upper- and middle-zone locations of parenchymal abnormalities
- Atypical features
– Lymphadenopathy: unilateral, isolated, anterior and posterior mediastinal.
– Airspace consolidation: masslike opacities, conglomerate masses, solitary pulmonary nodules, Confluent alveolar opacities (alveolar sarcoid pattern)
- Ground-glass and miliary opacities.
- Fibrocystic changes: cysts, bullae, blebs, emphysema, honeycomb-like opacities with upper- and Middle-zone predominance.
– Airway and pleural involvement.
Scadding staging of Thoracic Sarcoidosis
- This classification is based on chest X Ray and defines as stage I the presence of bilateral hilar adenopathy, stage II bilateral hilar adenopathy and pulmonary infiltrates, stage III pulmonary infiltrates without overt hilar adenopathy and stage IV the presence of overt pulmonary fibrosis.
References:
- Criado, E., Sánchez, M., Ramírez, J., Arguis, P., de Caralt, T. M., Perea, R. J., & Xaubet, A. (2010). Pulmonary Sarcoidosis: Typical and Atypical Manifestations at High-Resolution CT with Pathologic Correlation. RadioGraphics, 30(6), 1567–1586. https://doi.org/10.1148/rg.306105512
- Gaillard, F., 2021. Sarcoidosis | Radiology Reference Article | Radiopaedia.org. [online] Radiopaedia.org. Available at: <https://radiopaedia.org/articles/sarcoidosis-1> [Accessed 26 November 2021].
- Venkata Ramanan R, Pudhiavan A, Venkataramanan A. The “cluster of black pearls” sign of sarcoid lymphadenopathy: a new sign on thin-section contrast-enhanced multidetector CT. (2017) Clinical radiology. 72 (9): 729-736. doi:10.1016/j.crad.2017.03.031 – Pubmed
- Bernardinello, N.; Petrarulo, S.; Balestro, E.; Cocconcelli, E.; Veltkamp, M.; Spagnolo, P. Pulmonary Sarcoidosis: Diagnosis and Differential Diagnosis. Diagnostics 2021, 11, 1558. https:// doi.org/10.3390/diagnostics11091558
Dr. Deepti H V, MBBS, DMRD, DNB, EDiR
Consultant Radiologist
Manipal Hospitals Radiology Group.
Dr. Naveen SS, MBBS, MD
Cross Section Imaging Fellow
Manipal Hospitals Radiology Group.