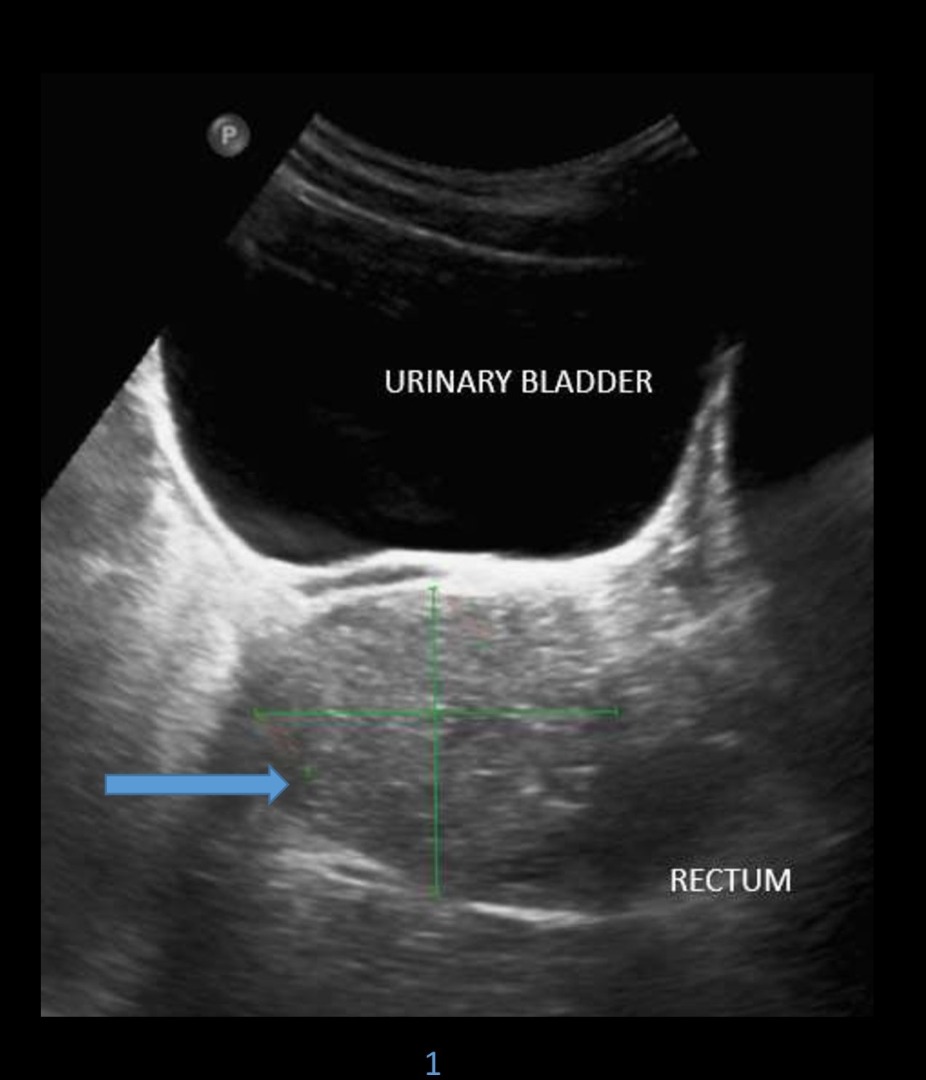
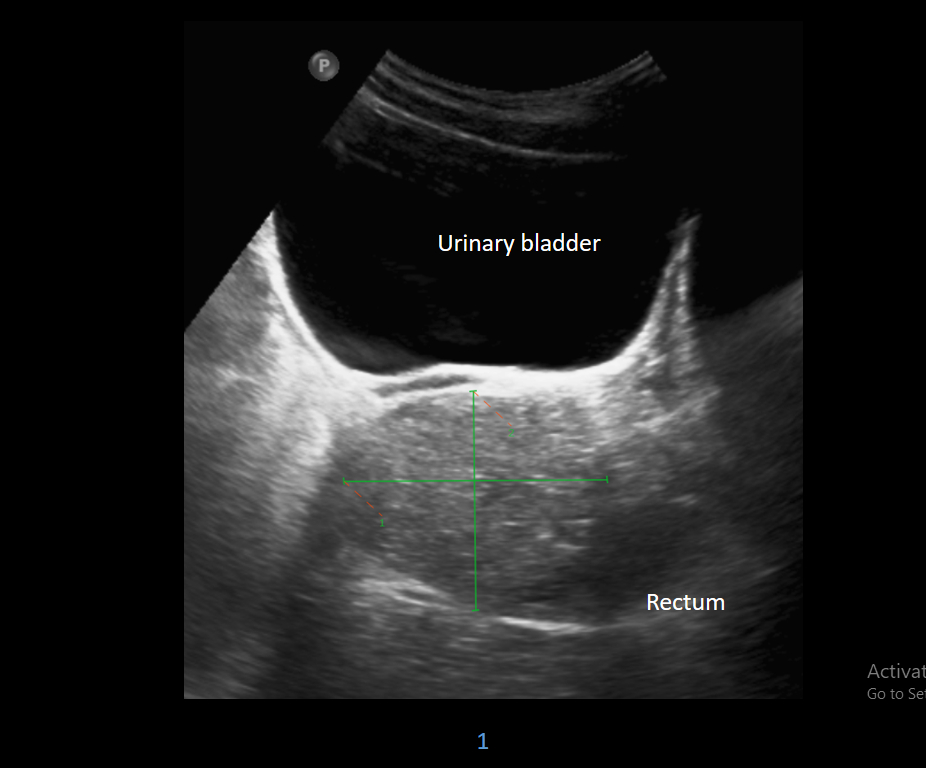
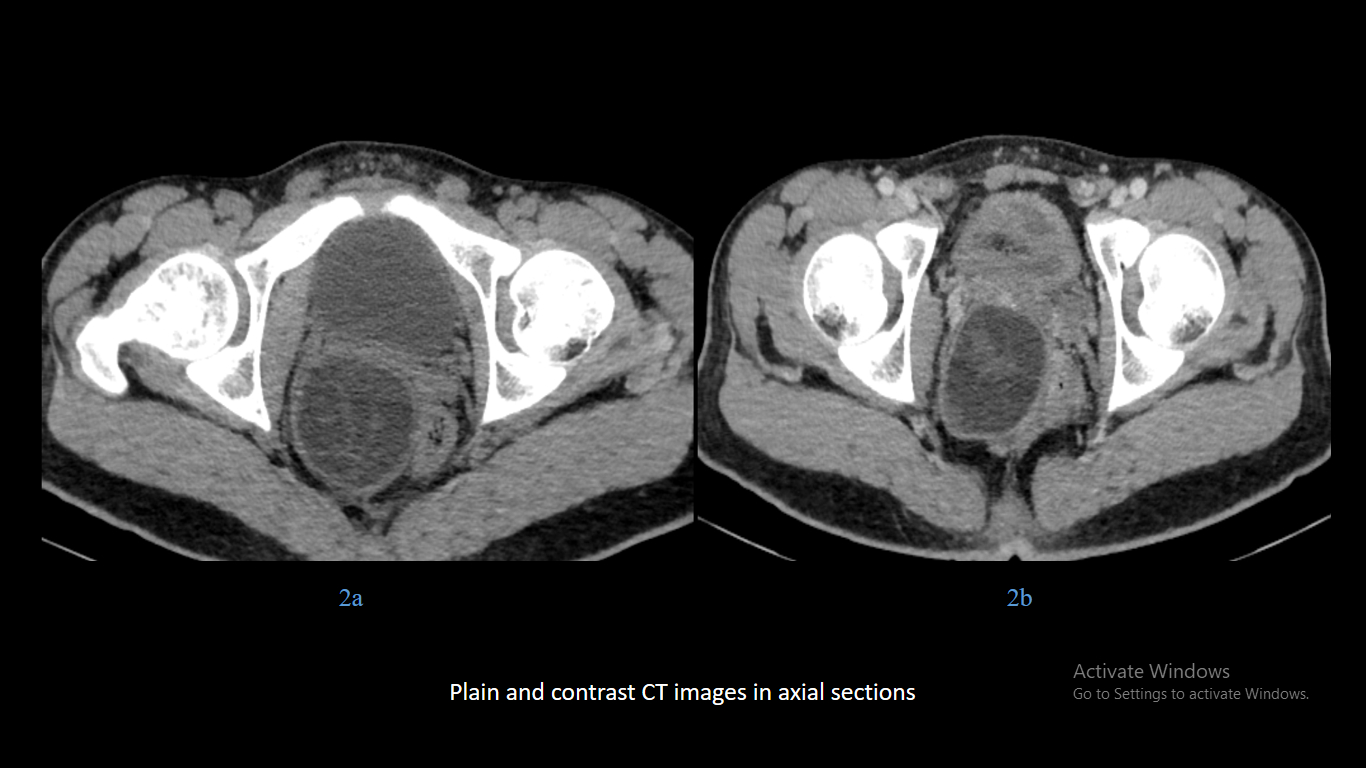
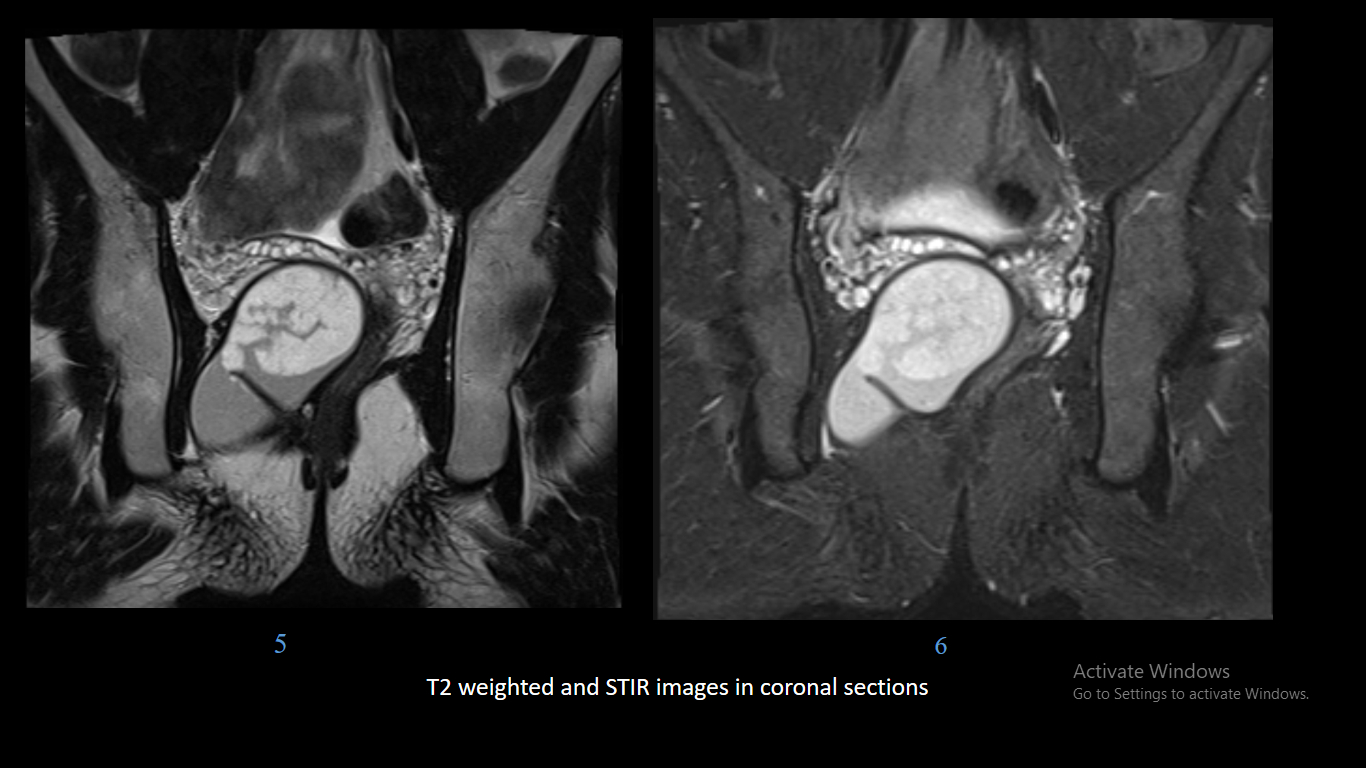
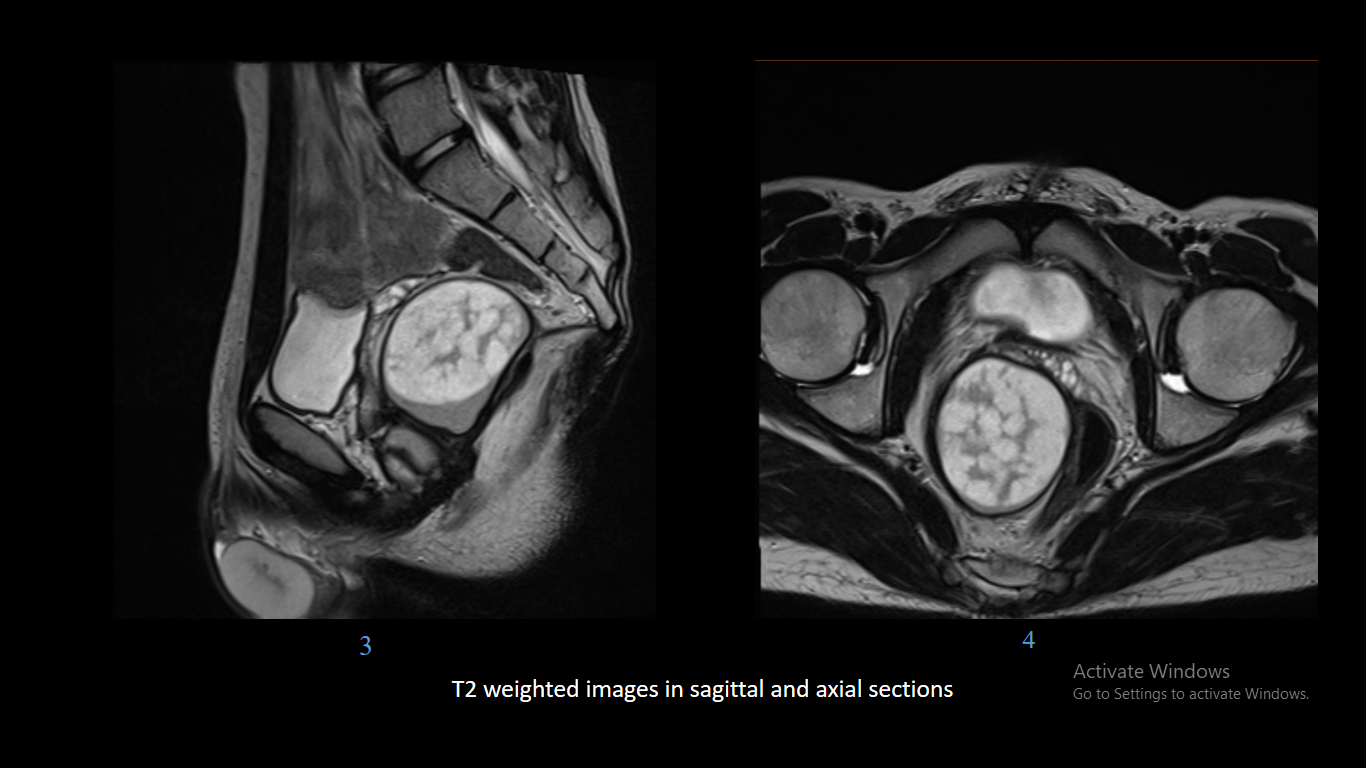
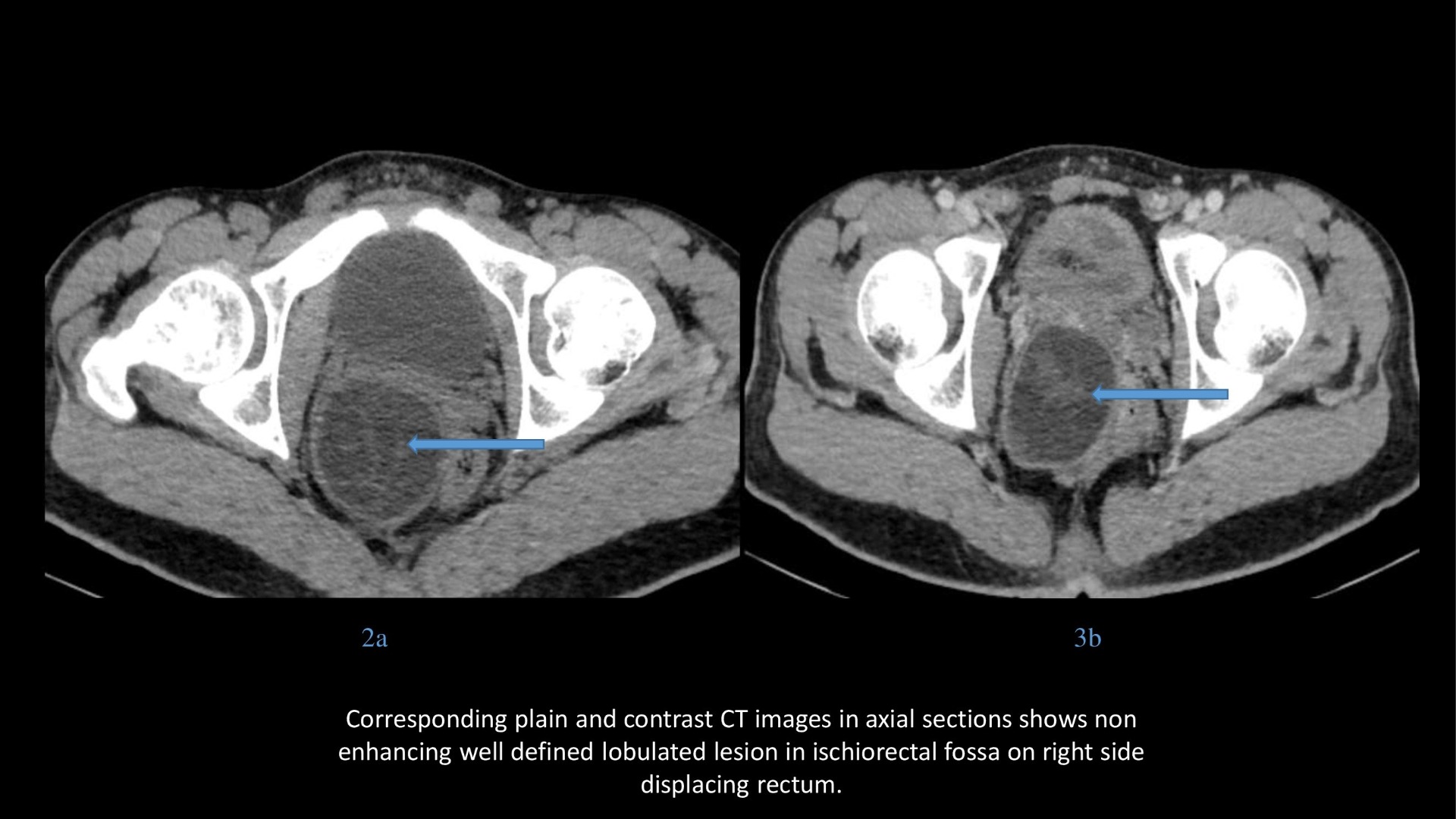
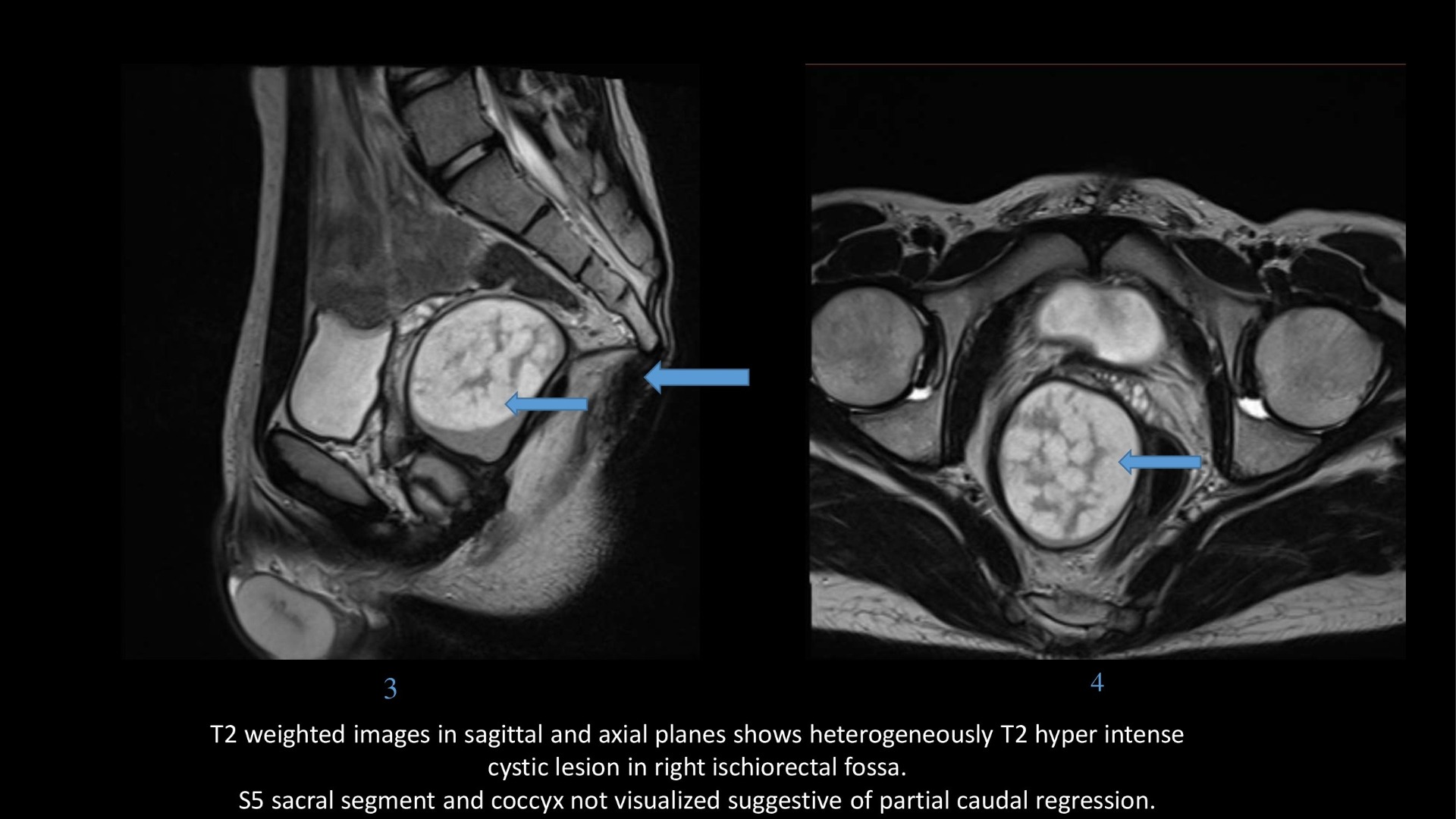
17 years male. History of abdominal discomfort and long-standing constipation.
Diagnosis
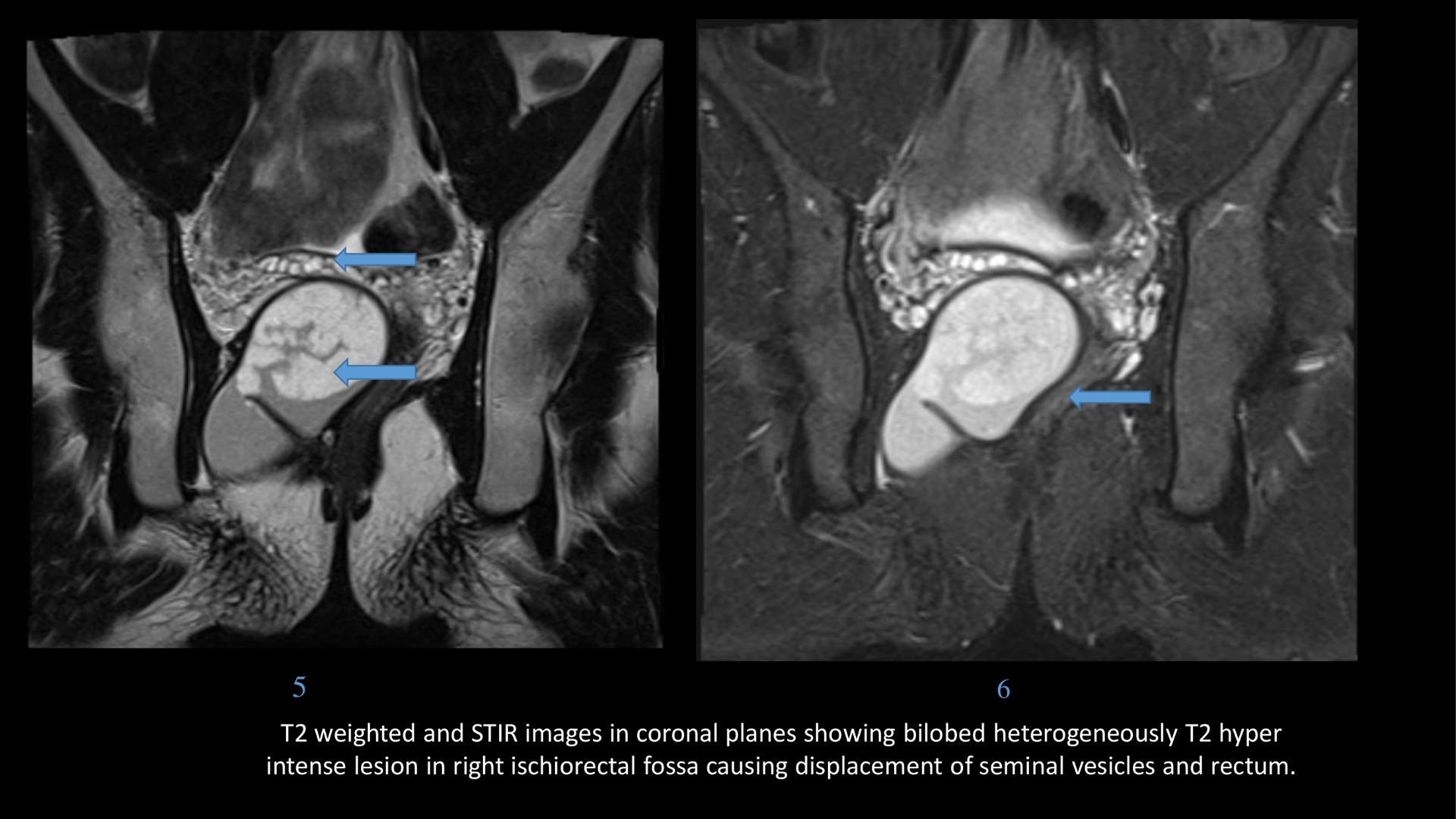
Pre sacral epidermoid cyst
Laparotomy with complete surgical excision of the cyst was performed. The histopathology confirmed the diagnosis of epidermoid cyst.
Discussion
Epidermoid cysts:
- Represent proliferation of squamous epithelium within a confined space.
- Either found incidentally or present as a firm non-tender lump.
- If they rupture a local inflammatory response to the necrotic debris released can mimic infection.
- Although they can be found anywhere, they are typically located on the scalp, face, neck, trunk, and back.
- Rarely epidermal cysts can undergo malignant degeneration with squamous cell carcinoma.
Pathology:
- They are thought to occur as a result of:
- Traumatic/surgical implantation.
- Occlusion of the pilosebaceous unit.
- Congenital rests of cells.
- Human papillomavirus type 57 or 60 infections implicated palm plantar epidermoid cysts.
Pre Sacral Epidermoid Cysts
- Developmental cystic lesions arising in the presacral location include dermoid cysts, epidermoid cysts, chordomas, adrenal rest tumors, anterior sacral meningoceles, cystic hamartomas, tailgut or rectal duplication cyst.
- Natural history of epidermoid cysts arising in the presacral region is elusive. Because of their unusual location and slow growth, they have a tendency to remain asymptomatic.
- Difficult to characterize on ultrasound and computed tomography.
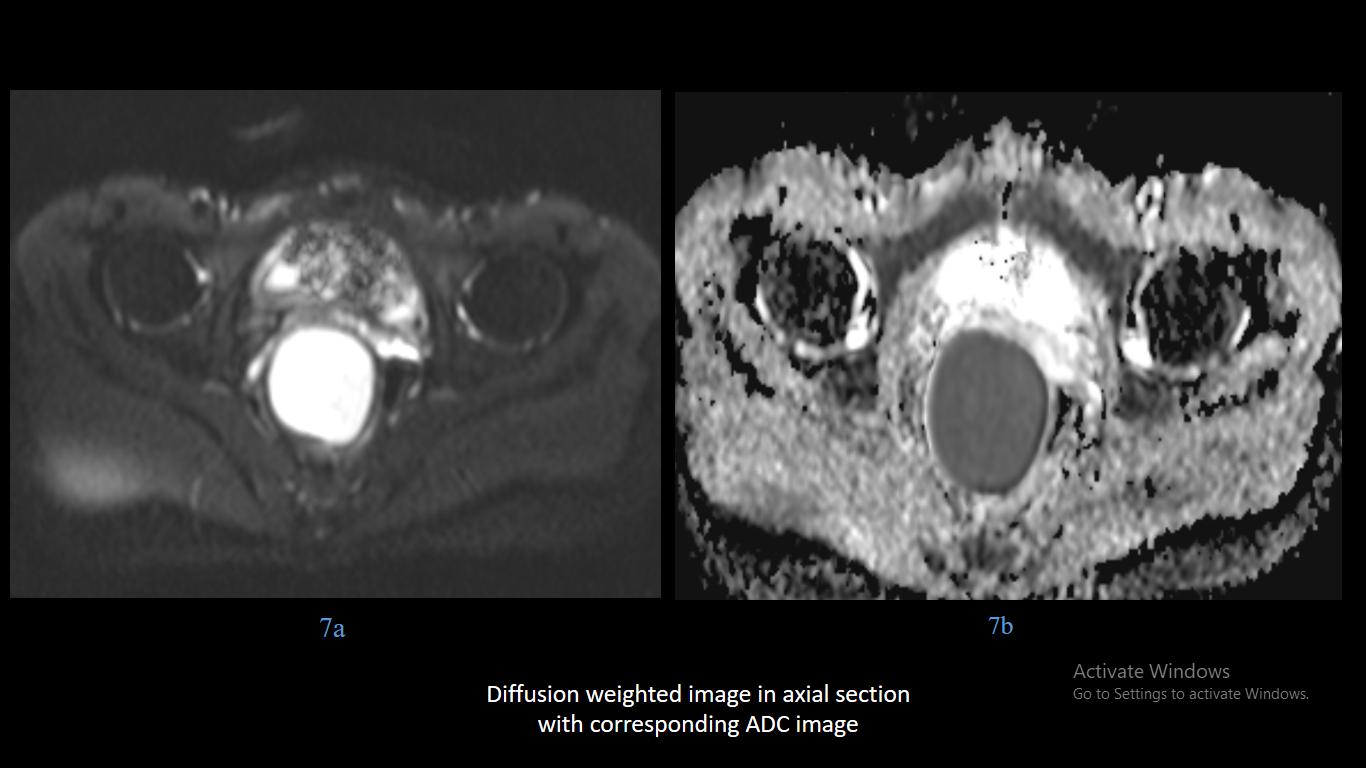
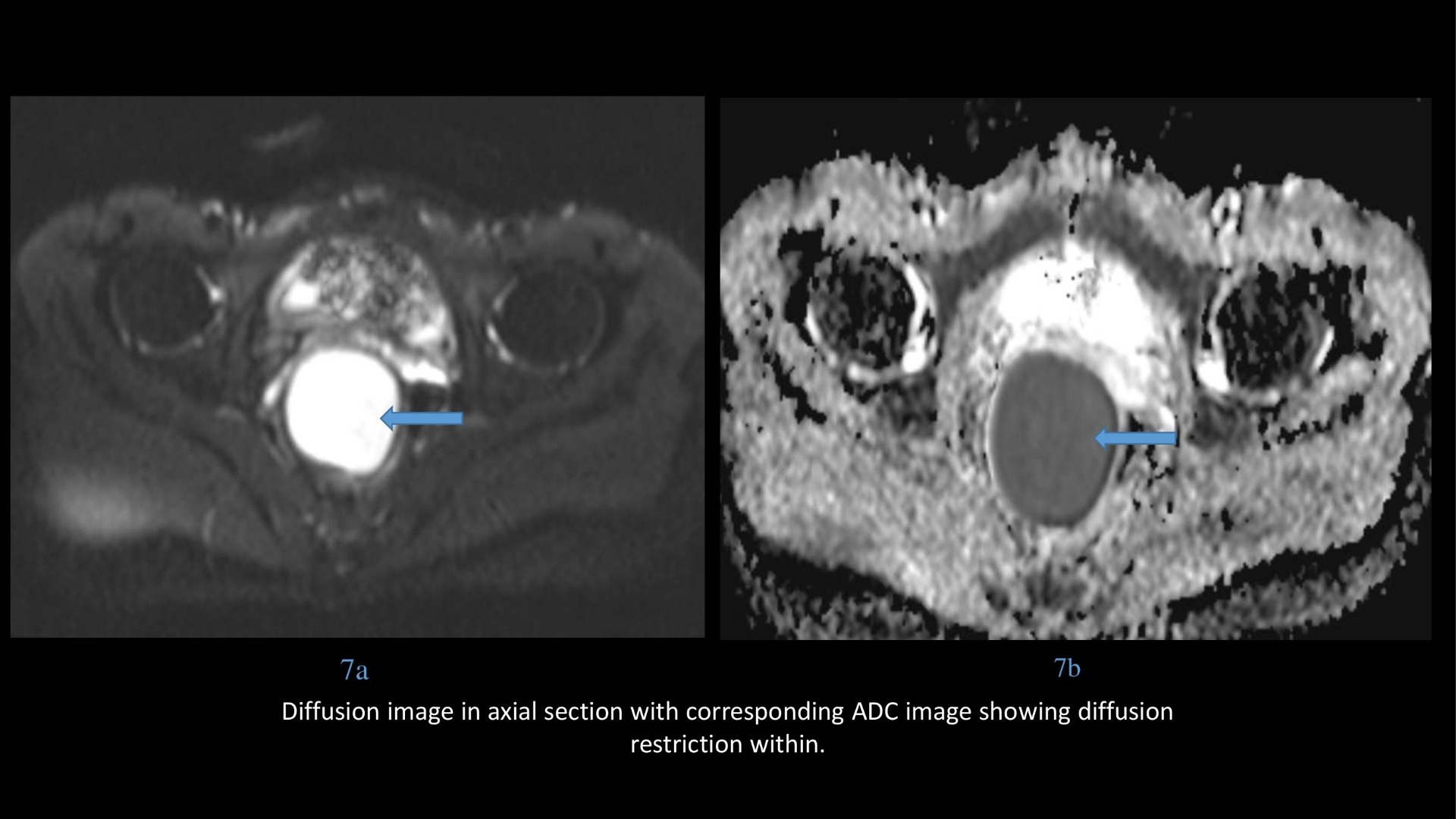
- MRI with the use of diffusion weighted imaging allows for definite preoperative diagnosis.
- Epidermoid cysts appear as T1 hypointense, T2 hyperintense masses which show diffusion restriction, wherever they are present within the body.
- T2 hypointense foci may be seen within the lesion because of presence of keratin.
- Another feature described in pre sacral epidermoid is differential restriction in contents of the cyst.
- MRI also helps differentiating between any bony, spinal canal or meningeal involvement, or signs of malignant degeneration.
- Heterogeneous signal intensity on T2, irregular thickened walls, solid component, and presence of enhancement are concerning for malignant change.
- A close differential of an epidermoid cyst on basis of diffusion restriction is a retrorectal pyogenic abscess. However abscess demonstrates presence of a thickened enhancing rim, intracavity fluid debris level or air specks; surrounding fat may show inflammatory changes with thickening of rectal wall.
Summary
- Presacral epidermoid cysts are unique in that they are the only developmental lesions that show diffusion restriction.
- MRI with diffusion weighted imaging allows for accurate differentiation of pre sacral lesions with good confidence thereby obviating the need of biopsy before surgery.
References
- U. Wollina, D. Langner, G. Tchernev, K. França, T. Lotti, Epidermoid cysts – A wide spectrum of clinical presentation and successful treatment by surgery: a retrospective 10-year analysis and literature review, Open Access Maced. J. Med. Sci. 6 (1) (2018) 28–30, https://doi.org/10.3889/oamjms.2018.027.
- H. Curtin, P. Som, Head and Neck Imaging, 4th ed., Mosby, 2002, pp. 2173–2183, https://doi.org/10.1016/S0720-048X(03)00181-5.
- Yang BL, Gu YF, Shao WJ, et al.: Retrorectal tumors in adults: magnetic resonance imaging findings. World J Gastroenterol. 2010, 14:5822-5829. 10.3748%2Fwjg.v16.i46.5822.
- Riojas CM, Hahn CD, Johnson EK: Presacral epidermoid cyst in a male: a case report and literature review. J Surg Educ. 2010, 31:227–232.
- Yang DM, Kim HC, Lee HL, et al.: Squamous cell carcinoma arising from a presacral epidermoid cyst: CT and MR findings. Abdom Imaging. 2008, 33:498-500. 10.1007/s00261- 007-9287-0.
- Izumi K, Tsutsumi S, Hara T, et al.: Large presacral epidermoid cyst in an asymptomatic woman. Radiol Case Rep. 2017, 12:738–740. 10.1016/j.radcr.2017.07.017
Dr. Srinivas P
Cross-sectional Fellow
Manipal Hospital Radiology Group (MHRG)
Manipal Hospital, Bengaluru.
Dr. Vishwanath Joshi
Consultant Radiologist.
Manipal Hospital Radiology Group (MHRG)
Manipal Hospital, Bengaluru.